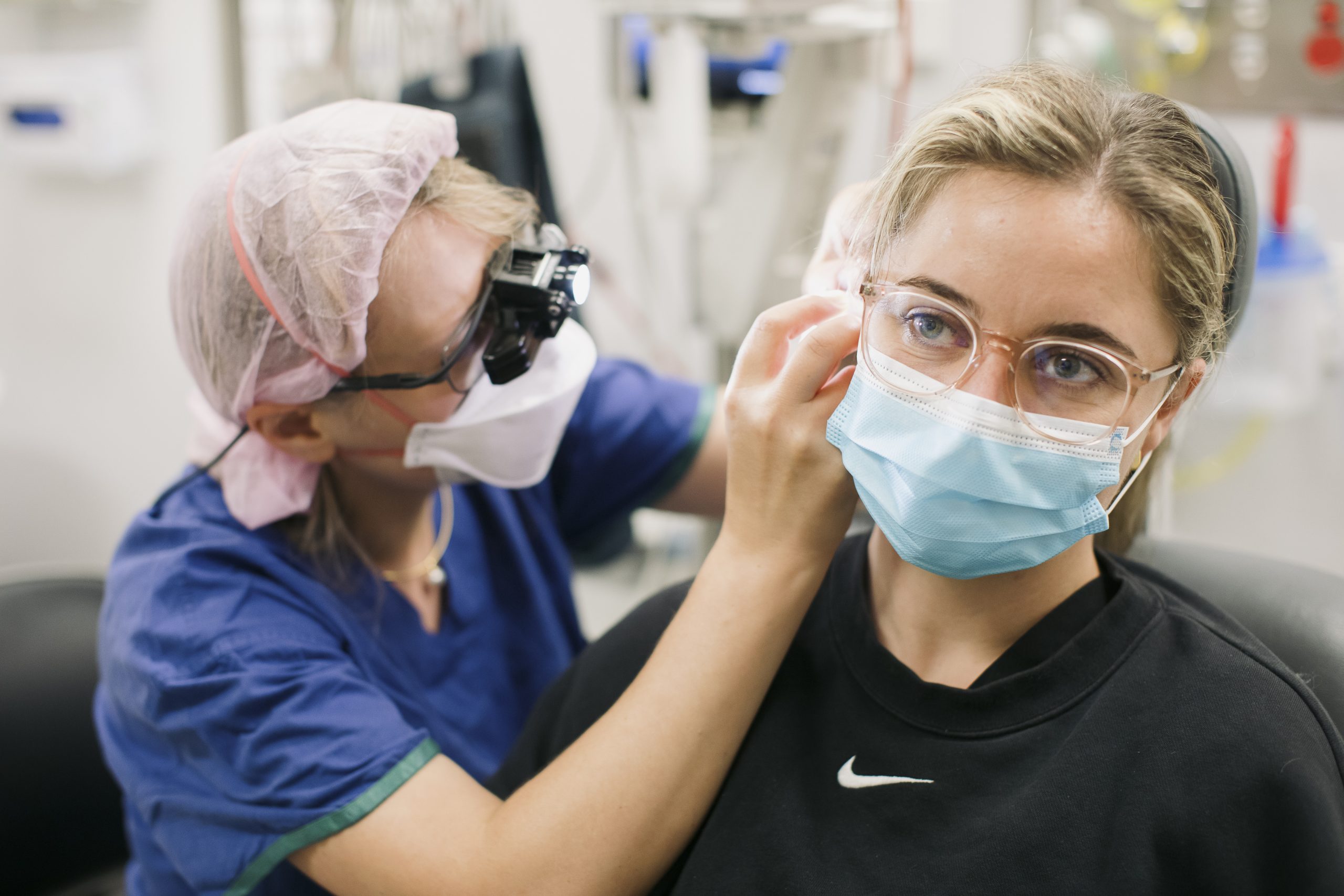
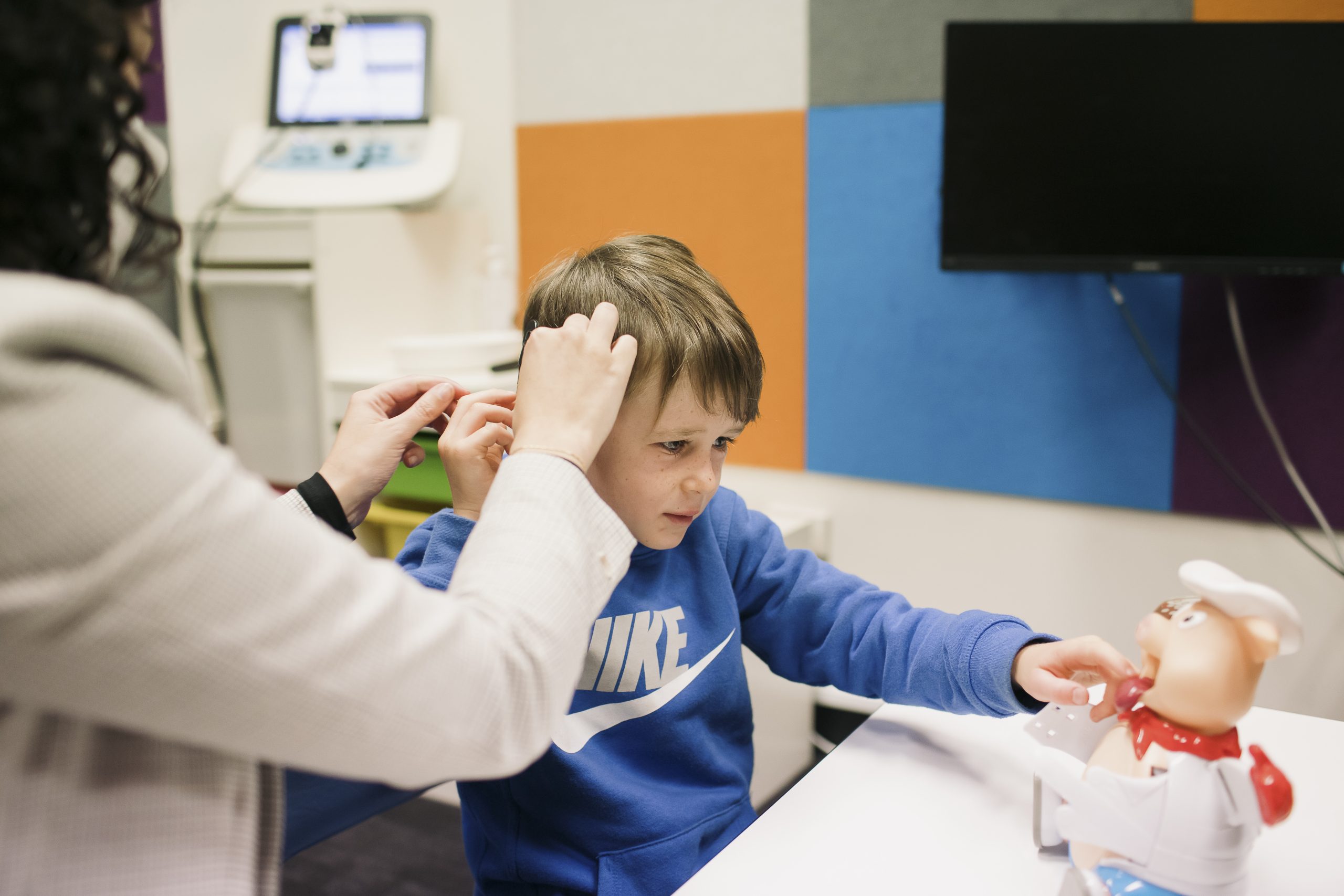
A new treatment being investigated for the hereditary eye condition Fuch’s Endothelial Dystrophy (FED) is improving patients’ vision without the need for a corneal transplant.
Fuch’s Dystrophy is a disease of the cornea – the clear front window of the eye – where cells in the corneal layer called the endothelium stop working. These cells normally pump fluid from the cornea to keep it clear but when they stop working, fluid builds up, the cornea swells, and vision becomes cloudy. Protein spots called guttatae also build up on the endothelium, degrading vision.
FED mainly affects people in their 50s and older. Often, people describe their vision as cloudy or hazy and the condition worsens until they gradually lose vision.
Patient Helen Aarons discovered her Fuch’s Endothelial Dystrophy (FED) while presenting at a routine optometrist appointment in early 2019. Helen was experiencing symptoms commonly attributed to cataracts, and she did in fact have cataracts, however Helen also had FED.
Currently, the only treatment is a corneal transplant where the diseased endothelial layer is removed and replaced with a donor cornea which has a healthy endothelial layer. This leads to an improvement in vision. FED is one of the most common reasons for a corneal transplant in Australia.
Ophthalmologists Associate Professor Elaine Chong and Dr Elsie Chan are leading a trial for a new treatment for FED at The Eye and Ear and Centre for Eye Research Australia.
They hope the new treatment, which enables the cornea to heal on its own, can become an alternative to a corneal transplant.
The new treatment involves an operation to remove a small area of unhealthy endothelial cells from the centre of the cornea. This encourages healthy endothelial cells from untouched areas of the cornea to move into the centre of the cornea, leading to recovery of the cornea.
“We remove a four-millimetre area of Descemet’s membrane along with its diseased endothelial cells, without inserting a corneal transplant,” Dr Chong explained. “This procedure is called Descemetorhexis Without Endothelial Keratoplasty (DWEK) or Descemet’s stripping only (DSO).”
Eye-drops involved in cornea endothelial cell healing – ‘rho-kinase inhibitors’ – are used in some cases that don’t heal on their own to encourage healthy endothelial cells to move to the centre of the cornea.
The Eye and Ear/CERA team has performed the procedure on 10 patients since the trial began in 2019. It was successful in eight, improving vision and avoiding transplant, while two whose endothelial cells failed to migrate centrally to clear their cornea required transplants.
Helen had her DWEK surgery in right eye in February 2021 and her recovery went well with the majority of her healing happening within the first month.
“DWEK had an 80 percent success rate in our trial with an improvement in visual acuity (clarity of vision) in all patients,” Dr Chong said. “It meant they achieved vision as if they had a transplant, but did not need a corneal transplant to do so, and stopped progression to blindness. It is too early to say if it is a cure, but it does improve vision. We will need to follow-up our patients for longer to see what happens in the long term,” Dr Chong said.
Helen was one of the successful participants and is now experiencing 20/20 vision in her right eye thanks to the DWEK procedure.
The best way to describe it is it is like watching an ultra HD TV in my right eye and then an old analogue TV in my left eye – the difference is extremely noticeable! At my most recent appointment, they told me I have the cornea of a 20 year old in my right eye,” Helen went on to say.
“A few other research groups have performed the procedure and have similarly found that DWEK can clear FED, but our study aims to recruit more patients and follow them for longer, for at least two years,” Dr Chong said.
“It is the best thing I’ve done for my eye health. The Eye and Ear staff have been wonderful and made my experience a really positive one. The outcome is much better than I ever imagined. If the procedure gets rolled out, I would book in my left eye in a heartbeat,” Helen explained.
“We are still refining our understanding to find which patients are suitable and who requires eye drops. More studies are needed to establish the clear role of DWEK in management of FED,” explained Dr Chong.